Dive Deeper
You are likely here because you’re curious about more significant life stressors or deeper forms of trauma, or because you yourself have had these experiences.
First, if you have experienced trauma, know that you are not alone and that there is nothing wrong with you. Our physical and mental reactions to chronic stress and trauma are normal responses to abnormal events.
Healing from trauma is a process, not a destination.
Your primary job is to be gentle with yourself and to take one small, safe step at a time.
Stress and the Nervous System
Stress is a good thing and necessary for human survival. Without mental and emotional stress, you would lack the understanding of how to survive in your environment or with groups of others. Without the physical stress of gravity and physical activity, your bones and muscles would not develop.
Because stress is a normal and necessary part of being human, our bodies have a finely tuned and adapted method for handling stressful experiences in our environment. The nervous system is the primary bodily system responsible for initiating, coordinating, and managing our mental and emotional response to stress.
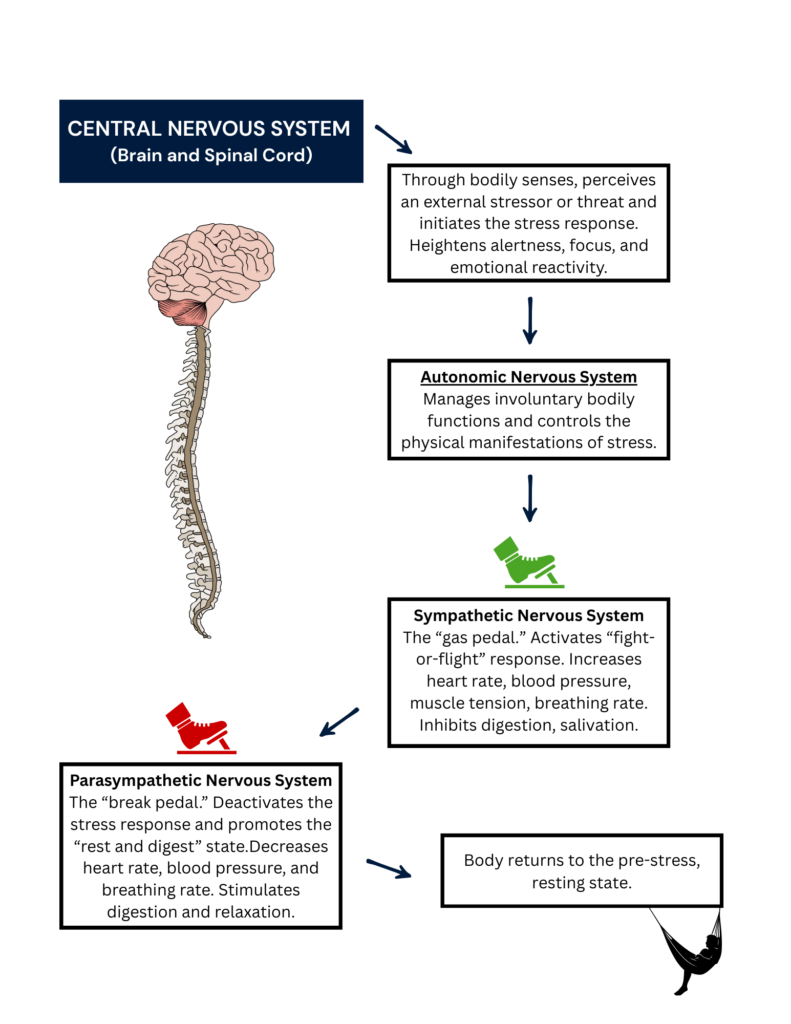
A healthy nervous system is able to experience stressors and move through a heightened state of arousal without getting “stuck” pushing down our internal gas pedal. It’s also able to stay balanced when the body works to slow itself back down by hitting the breaks, easing off of them once the body has returned to calm.
However, just like too much pressure can break a bone, too much mental and emotional pressure causes chronic stress or trauma, leading to a dysregulated nervous system. This dysregulation causes the body to get stuck with either the gas pedal down or the break pedal down, or on a roller coaster of extreme ups and downs between the two.
Understanding Differences in Stress, Chronic Stress, and Trauma
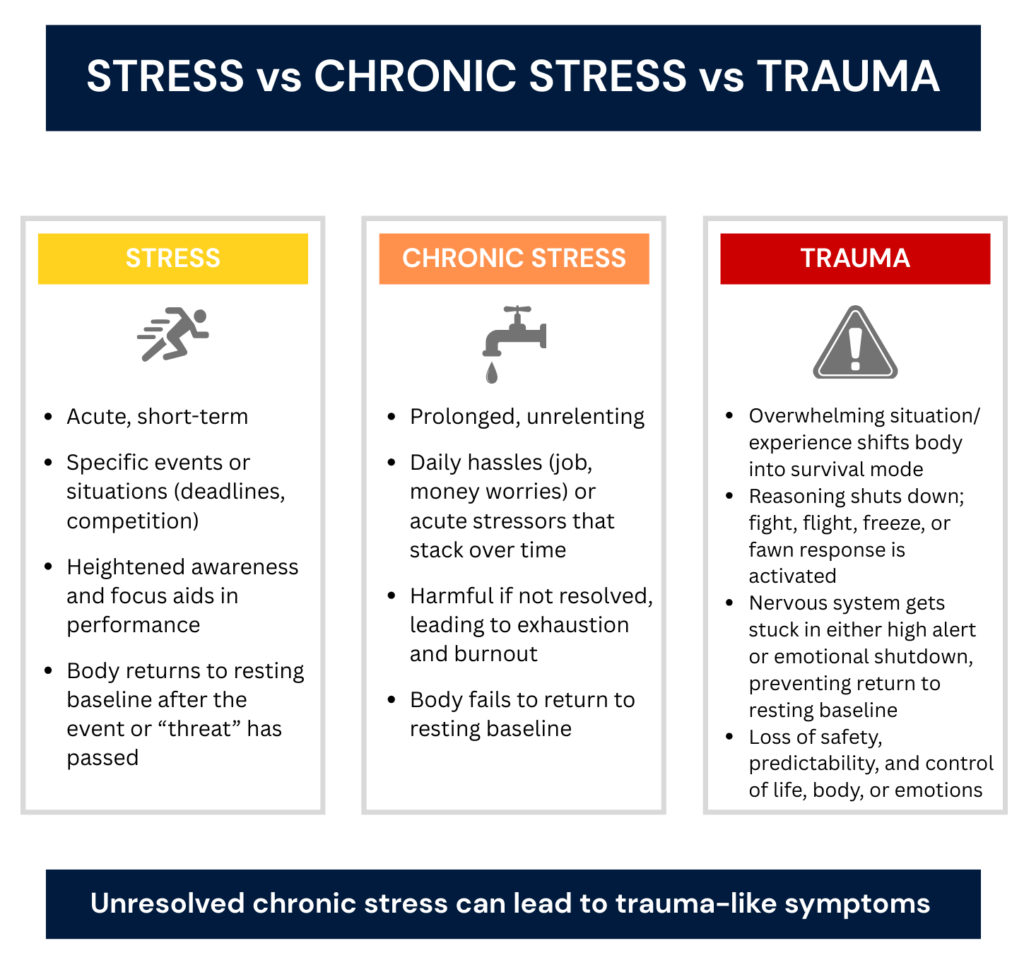
Transformation of Chronic Stress Into Trauma
When we talk about chronic stress accumulating, we are primarily referring to the physical and chemical toll it takes on the body, especially the brain’s alarm system.
The mechanism by which chronic stress turns toxic is called Allostatic Load.
- Allostatic Load is the cumulative “wear and tear” on the body systems that results from being constantly in allostasis.
- Allostasis means “achieving stability through change.” It is the process of the body constantly adjusting its stress hormones (like cortisol) and blood pressure to meet demands. In other words, being in allostasis is like trying to maintain an average speed by alternating slamming on the gas and going fast, with slamming on the breaks and going slow.
When the body experiences too much Allostatic Load, the stress response system breaks down. In other words, this continual “whiplash” creates trauma in the nervous system. This leads to trauma-like symptoms like:
- Stress Hormone Overdrive: The body becomes hyper-sensitized to threat. The amygdala (the brain’s alarm center) becomes overactive, while the prefrontal cortex (logic/reasoning center) weakens.
- Physical Exhaustion: Continuous production of adrenaline and cortisol drains the system, leading to burnout, immune suppression, and physical health problems.
When this chronic hyper-arousal continues, the brain begins to function as if it is constantly under attack, mirroring the symptoms of Post-Traumatic Stress Disorder (PTSD).
| Trauma Symptom | How Chronic Stress Causes It |
| Hypervigilance | Instead of looking out for a tiger, you are constantly scanning for a critical email, an angry phone call, or a financial deadline. Your nervous system is perpetually on high alert. |
| Emotional Numbing/Dissociation | The sheer volume of stress becomes too much for the conscious mind to process, leading to emotional detachment, feeling “checked out,” or difficulty feeling joy (a classic trauma response). |
| Irritability and Emotional Reactivity | With the prefrontal cortex weakened by chronic cortisol, the emotional regulation center breaks down. Small annoyances (a loud noise, someone cutting you off) trigger disproportionately strong “fight” or “flight” reactions. |
| Sleep Disturbances | The hyper-aroused nervous system interferes with the body’s ability to enter deep rest (parasympathetic mode), leading to chronic insomnia, nightmares, or disrupted sleep patterns. |
Trauma-Informed Self-Care and Lifestyle Practices
Trauma leaves a physiological footprint, often keeping the body’s nervous system (specifically the sympathetic nervous system, or “fight/flight”) hyperactive. Effective self-care focuses on consistently signaling safety to the body to activate the parasympathetic nervous system (the “rest and digest” state).
Movement and Physical Release
Movement is vital for trauma healing because traumatic stress is often described as “incomplete action” where the body prepared to fight or flee but was unable to complete the action. The residual energy (adrenaline, cortisol) gets trapped.
| Practice | Why It Helps with Trauma | Example Techniques |
| Gentle, Rhythmic Exercise | Rhythmic and predictable movement helps regulate the nervous system and can gently move the body out of freeze/immobility states. | Walking, cycling, swimming, or using an elliptical machine. The key is rhythm, not intensity. |
| Trauma-Informed Yoga/Somatic Practice | Focuses on interoception (awareness of internal body signals) and choice. It often avoids positions that feel triggering or restrictive. | Simple, repetitive poses (cat-cow, child’s pose), and noticing without judgment how the body feels. |
| Shaking/Vibrating | Directly releases trapped muscle tension and hormonal energy, which is a natural mammalian response to threat (e.g., animals shake after a narrow escape). | Shake your arms and legs vigorously for 30 seconds, or engage in practices like Tension and Trauma Releasing Exercises (TRE). |
Mindfulness and Grounding Techniques
Trauma pulls the mind either backward (into memory, flash, or intrusive thoughts) or forward (into hyper-vigilance and prediction of future threats). Grounding brings the attention back to the current, safe reality.
- The 5-4-3-2-1 Technique: This is one of the most effective grounding methods. It quickly interrupts dissociation or overwhelming emotional states by engaging the senses:
- 5 things you can see.
- 4 things you can touch (or feel).
- 3 things you can hear.
- 2 things you can smell.
- 1 thing you can taste (or a positive affirmation, such as “I am safe now”).
- 5 things you can see.
- Mindful Breathing: Focusing on slow, deep, diaphragmatic breaths. Slowing the exhale (making it longer than the inhale) is a direct signal to the vagus nerve that you are safe.
- Body Scan: Briefly noticing where your body is contacting a chair, the floor, or the ground, reaffirming your connection to the present reality.
Connection and Social Engagement
Trauma often involves relational betrayal or isolation, leading to chronic feelings of being unsafe around others. Repairing this sense of safety requires safe connection.
- Identifying “Safe” People: Deliberately choosing to spend time with people who are reliable, non-judgmental, and who respect your boundaries.
- Co-Regulation: The nervous system regulates best when it is around another regulated nervous system. Spending time with a calm, trusted friend (even silently) can help your own system settle.
- Community: Engaging in group activities that are low-pressure (e.g., a craft class, a book club) to rebuild a sense of belonging and shared human experience.
Establishing Predictable Routine
A central component of trauma is unpredictability and loss of control. Reintroducing structure and routine creates an environment of psychological safety.
- Sleep Hygiene: Trauma severely disrupts sleep. Maintaining a consistent bedtime and wake-up time, and creating a calming routine before bed, helps the body achieve deeper restorative rest.
- Nourishment and Hydration: Eating regular, balanced meals prevents extreme blood sugar drops, which can mimic or trigger anxiety and panic symptoms.
- Daily Rhythms: Having predictable times for waking, working, eating, and relaxing reinforces the message that life is orderly and that you are in control of your time.
The Importance of Pacing and Choice
In all these practices, two principles are paramount:
- Pacing: Never rush the process. If a technique (like deep breathing or a yoga pose) triggers a feeling of panic or dissociation, stop immediately. Healing must happen at a pace that feels safe and manageable.
- Choice: A loss of choice is often a core element of trauma. All self-care should be presented as an experiment or an option. The ability to say “no” or change your mind is essential for empowering the individual and restoring agency.
Additional Resources
These organizations offer free, evidence-based information, additional toolkits, and educational materials on stress, trauma, and mental wellness.
- The National Center for PTSD (U.S. Dept. of Veterans Affairs), https://www.ptsd.va.gov/
- Focus: Trauma, coping skills, and evidence-based treatments.
- Resources: They offer self-help guides for coping with stress reactions, and mobile apps like Mindfulness Coach and PTSD Coach which provide immediate coping skills.
- The National Child Traumatic Stress Network (NCTSN), https://www.nctsn.org/
- Focus: Provides clear definitions of trauma, stress, and toxic stress, with resources tailored for various age groups.
- Resources: Excellent fact sheets and toolkits on trauma-informed care and building resilience.
- The Substance Abuse and Mental Health Services Administration (SAMHSA), https://www.samhsa.gov/
- Focus: Broad mental health and substance abuse resources, with a strong focus on Trauma-Informed Approaches.
- Resources: Their concepts and guidance documents explain the core principles of a trauma-informed perspective (Safety, Trustworthiness, Collaboration, etc.).
- Centers for Disease Control and Prevention (CDC), https://www.cdc.gov/mental-health/living-with/index.html
- Focus: Managing stress and promoting mental health, with practical tips on lifestyle factors like sleep, exercise, and diet.
These books are considered foundational in understanding the body-mind connection in trauma and chronic stress. They are excellent places to learn more
| Book Title | Author | Core Focus & Why It’s Recommended |
| The Body Keeps the Score | Bessel van der Kolk, M.D. | Trauma & Neuroscience. Considered the definitive resource. Explores how trauma literally reshapes the brain and body and reviews different healing modalities (e.g., Yoga, EMDR, neurofeedback). |
| Waking the Tiger: Healing Trauma | Peter A. Levine | Somatic Healing. Introduces Somatic Experiencing (SE), an approach that focuses on the body’s natural capacity to heal trauma by processing physical sensations and regulating the nervous system. |
| What Happened to You? | Bruce Perry, M.D., Ph.D. & Oprah Winfrey | Childhood Trauma & Resilience. Focuses on shifting the perspective from “What’s wrong with you?” to “What happened to you?” Explains brain development and the impact of Adverse Childhood Experiences (ACEs) in an accessible, conversational format. |
| My Grandmother’s Hands | Resmaa Menakem | Intergenerational & Racialized Trauma. Blends somatic practices with a historical understanding of trauma, urging readers to heal through body-focused methods rather than solely cognitive approaches. |
| The Deepest Well | Nadine Burke Harris, M.D. | ACEs & Chronic Disease. Explores the profound link between childhood adversity (trauma/toxic stress) and long-term physical health issues, including chronic illnesses. |